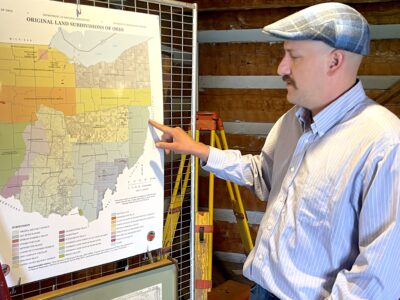
Hampton founds area’s first pure direct primary care

Mirror photo by William Kibler / Illustration by Nick Anna Dr. Sean Hampton’s Hampton Medical: Direct Primary Care is the first “pure” DPC practice between Harrisburg and Pittsburgh. The service charges a monthly subscription fee rather than depending on patient insurance for compensation.
Editor’s note: This is the third in a three-part series.
By William Kibler
bkibler@altoonamirror.com
ou can watch the old “Marcus Welby, MD” shows now on Amazon Prime.
The pairing of that 1970s TV drama with the modern monthly subscription service helps illustrate how a local primary physician wants to help revive the traditional family doctor model embodied by Welby by using the newfangled payment model embodied by the streaming video services — in hopes of contributing to the cure of one insurance-dependent sector in our ailing health system.
Dr. Sean Hampton’s Hampton Medical: Direct Primary Care, the first “pure” DPC practice between Harrisburg and Pittsburgh, charges a monthly subscription fee, like Prime or Netflix, rather than depending on patient insurance for compensation.
It doesn’t make sense to pay for a GP — or general practitioner’s — often-routine checkup and problem-solving with insurance, any more than it would make sense to pay for oil changes with car insurance, said Hampton, echoing a frequently used argument for DPC, which is growing nationally, with about 1,000 practices in 48 states and Washington, D.C.
It does make sense, however, to pay for primary care through monthly subscriptions, according to Hampton. Among the benefits: It helps ensure continuity of care, eliminating the need for tests that might be needed when a doctor is unfamiliar with a patient and opening up avenues for consultation like voice, video, text and email — methods which insurance plans don’t pay for, Hampton said.
Smaller patient roster
With insurance creating lots of overhead for primary care practices, young doctors burdened with student debt, the Affordable Care Act mandating the use of extensive patient exam checklists and an existing shortage of family doctors, primary care has become so unappealing that many newly trained in family practice are going into other specialties, aggravating the shortage and further burdening doctors who remain — reducing even further the time they can spend with patients, according to Hampton.
By contrast, the DPC model allows for a smaller patient roster — 750 versus 2,500 to 5,000 — so the DPC doctor can spend the time necessary to prevent problems and manage chronic diseases like diabetes, according to Hampton.
“To move the needle at all (for such chronic conditions), you need to talk about diet, exercise, lifestyle, nutrition and medications,” Hampton said.
The DPC approach seeks quality rather than quantity, said Hampton’s fiance and office manager Maya Waide.
One of the key advantages of the traditional relationship between family doctors and their patients is continuity, according to Hampton.
“I’m trying to bring it back,” he said.
It’s “ridiculous” that patients, even with good insurance, can’t get an appointment with their doctor when they need it, he said.
Because of their smaller rosters, DPC doctors can grow familiar with each of their patients, based on initial lengthy visits, which, ironically, will enable those doctors to deal with many later problems with those patients by voice or video phone, text or email, with and prescriptions called in by the doctor to a pharmacy or medications picked up at the DPC office, according to Hampton.
If a patient has a urinary tract infection and can describe the symptoms over the phone, and those infections recur several times a year, the DPC doctor won’t need to summon the patient into the office to prove to an insurance company that the patient has a UTI — as there is no insurance involved, Hampton said.
Upper respiratory tract infections and flu are other maladies for which the doctor may not need to see patients who can answer several standard questions about their symptoms, Hampton said.
Patients whose blood pressure medicine has been changed may not need to return to the office in the standard two weeks, because they can take their own pressure readings at home and send them in, Hampton said.
Likewise, stabilized diabetics can text or email a list of what they’ve been eating and blood sugar levels for the past two weeks for any recommended adjustments, he said.
About 30 percent of all primary care visits can safely be eliminated this way, he said.
Actually, a much higher percentage — 70 to 80 percent — can be eliminated this way, “once a health care plan has been established,” according to Mark Tomasulo, founder of PeakMed, cited in an article from the Medical Group Management Association.
Citing advantages
Getting to know patients better can help make diagnoses more incisive, according to Hampton.
If a young person comes to a primary care office with bad headaches and other alarming symptoms, a rushed doctor unfamiliar with the patient may reflexively order an MRI, according to Hampton.
A DPC doctor might have enough familiarity with that patient to figure out that the problem is actually the result of stress from the patient’s mother-in-law having recently come to live with the family, Hampton said.
Not all diabetes, thyroid and orthopedic issues need to result in a referral to a specialist, if the primary care doctor spends enough time, he said.
Having time to pay more attention to each patient also can lead to prescribing fewer medications, and controlling diabetes, chronic pain, fibromyalgia and other conditions through better nutrition, proper rest and exercise, Hampton said.
“What’s easier — to talk to someone about their problems for 25 minutes or prescribe an antidepressant after talking to them for three?” he asked rhetorically.
A DPC doctor can also coordinate specialist care, helping reduce confusion, Hampton said.
Sometimes, when patients don’t understand what specialists say about problems like kidney ailments, diabetes and cardiac issues, Hampton can call those specialists, then interpret for the patients, he said.
Critics who believe DPC advocates make grandiose claims point out that the model is limited to primary care issues.
That’s true, according to Dr. Paul Thomas of Plum Health Direct Primary Care in Detroit.
But the DPC model allows primary care doctors to exploit all their knowledge, with the time to spend with patients, time denied to primary doctors by the modern, insurance-based model, Thomas said.
“When a well-trained family medicine doctor is able to practice at the top of their training, they are able to manage between 80 and 90 percent of all patient concerns,” Thomas said.
“If I have an hour, I can use it to drain an abscess, to talk about the efficacy of your anti-depressants, to draw your blood for the lab work you need, to remove that ingrown toenail, to fully evaluate your vertigo, to evaluate your child’s Vanderbilt scores for ADHD, to dispense the necessary medications and more,” Thomas wrote. “In the current fee-for-service system, the expectation is that primary care doctors perform a cursory evaluation and then make a referral to a specialist.”
Insurance vital cog
While DPC isn’t “trying to be a global solution,” it can nevertheless help reduce the need for speciality care, emergency room visits and hospitalization, which is why it can be important for DPC patients to carry insurance for occasions when such further care is needed, DPC physical Rob Lamberts wrote.
Seeing the doctors under whom they train demoralized by heavy caseloads forced on them by administrative pressure, many recent medical school graduates in primary care are opting for other specialities, Hampton said.
Some take “pretty cushy” jobs as hospitalists, and others go into urgent care, where they can earn more than $200,000 a year, Hampton said.
There are traditional family practices that do well financially on 10 to 15 patients a day, but those are generally run by older, established doctors with good retirement plans, money in the bank and no student loans to repay, according to Hampton.
As it is now, a third of his paycheck goes into student loans, he said.
Critics say that the expansion of DPC has the potential to worsen the primary care doctor shortage, because DPC rosters are much smaller.
The critics call it “patient abandonment,” stated Thomas in a blog post on the practice’s website.
But insofar as DPC creates a more attractive kind of primary care, it could encourage young primary doctors to remain in family care and older ones to put off retirement, Hampton said.
Critics also accuse DPC of being elitist, Lamberts said in an article in Medical Economics. But since moving to DPC from a 3,000-patient traditional practice, Lamberts has served a lower-income patient group, he wrote.
“There are more self-employed, uninsured and even unemployed patients,” Lamberts wrote. “I think it is the predictability and transparency of cost that makes DPC appealing.”
DPC can ultimately help reduce health care costs, as overhead for a DPC office is about 35 percent of the total revenue stream — compared to 65 percent for a typical primary care office, Hampton said.
That overhead is lower largely because there are “No third parties or Fee for Service billing to inflate costs,” states dpcare.org.
It’s also lower because he can handle many consultations without seeing patients in person, Hampton said.
Patients’ savings
Patients, too, can realize savings, as a study by Qliance of Seattle showed that DPC subscribers saved about 40 percent on their medical expenses, Hampton said.
DPC also can reduce costs for patients by taking care of problems like diabetes and hypertension “before they become serious,” Lamberts wrote.
DPC simplifies the “access point” into the health care system for patients, while helping eliminate confusion in connection with other aspects of health care — although to say it simplifies health care in general is an overstatement, according to Hampton.
Hampton’s practice might seem to be at risk from patients whose medical problems tax his time and efforts far in excess of their subscription payments, but “it all balances out,” he said.
His practice might also seem to be at risk from patients inclined to abuse the unlimited consultation to which their subscriptions entitle them, but a talk to re-establish boundaries should fix that, he said.
All attempts so far to fix the health care system in the U.S. have been “top down,” insurance-based and regulatory, according to Hampton. The ACA is an example of that, he said.
DPC — while “not a panacea” — is “innovation from the bottom,” a provider-based fix that
doesn’t involve insurance for one portion of the health care system that is “kind of broken,” Hampton said.
Mirror Staff Writer William Kibler is at 949-7038.